As spinal surgery becomes more advanced, so do the methods used to control postoperative pain. Dr. Larry Davidson, an expert in spinal surgery, explores how pain pumps, also known as intrathecal or Patient-Controlled Analgesia (PCA) systems, offer an effective solution for managing pain immediately after complex procedures. These devices deliver medication directly where it’s needed, minimizing systemic side effects and providing targeted relief during the most critical phases of recovery.
Pain pumps have become an important tool in modern recovery protocols, offering more precise control over pain while reducing the reliance on high-dose opioids.
What are Pain Pumps?
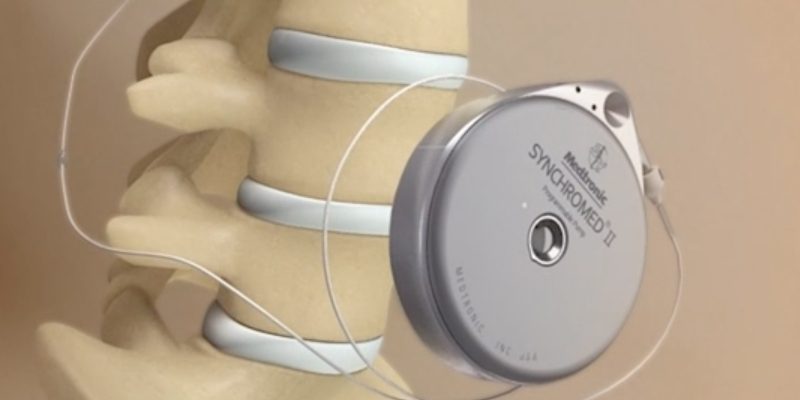
Pain pumps are medical devices that deliver pain-relieving medication directly to the spinal cord or surrounding tissue through a catheter. They are typically used in the hours or days following spine surgery to manage acute pain. These pumps can be external or implanted and are often filled with medications such as morphine, fentanyl or local anesthetics like bupivacaine.
By delivering medication straight to the source of pain, these systems allow for lower overall dosages while maintaining strong analgesic effects. Some pain pumps are continuous, while others allow patients to control the timing and amount of medication with the push of a button.
Advantages of Pain Pumps in Spine Surgery Recovery
The use of pain pumps offers several notable benefits:
- Targeted relief: Because medication is delivered directly into the spinal space, patients often experience faster and more consistent pain control.
- Reduced systemic exposure: Lower medication doses mean fewer side effects like drowsiness, nausea or constipation.
- Improved mobility: Better pain control allows patients to begin moving earlier, reducing risks such as blood clots and muscle atrophy.
- Customizable dosing: Patient-controlled systems provide autonomy and flexibility in managing pain levels during activity or rest.
These benefits are especially valuable in complex procedures like spinal fusions, scoliosis corrections or multi-level decompressions where inflammation and nerve irritation are prominent.
Common Use Cases for Pain Pumps
Pain pumps are most commonly used after major spinal surgeries, particularly when traditional oral medications may not provide adequate relief. They are also beneficial for:
- Patients with high opioid tolerance: Those who take opioids regularly before surgery may need higher doses for the same effect. Pain pumps help by providing localized delivery without overburdening the body’s systems.
- Patients undergoing extensive hardware placement: These procedures can cause significant post-surgical discomfort, which is more effectively managed through targeted administration.
- Patients who are sensitive to systemic opioids: Individuals prone to gastrointestinal issues or respiratory complications may benefit from a more localized approach to pain relief.
By addressing pain at its source, pain pumps support a smoother and often faster recovery process, especially in the critical first few days after surgery.
Dr. Larry Davidson remarks, “Emerging minimally spinal surgical techniques have certainly changed the way that we are able to perform various types of spinal fusions. All of these innovations are aimed at allowing for an improved patient outcome and overall experience.” This alignment of surgical innovation with advanced pain control strategies, like pain pumps, reflects a growing focus on optimizing both safety and comfort in the immediate postoperative period.
Types of Pain Pumps and Delivery Methods
There are two primary types of pain pumps used in spinal surgery recovery:
- External pumps: These are connected to a catheter placed in or near the spine and are removed after a few days. They are commonly used in hospitals during the early post-op period.
- Implantable pumps: Typically used for chronic pain, these are placed under the skin and programmed to deliver medication over a longer period. While not common in routine post-op care, they are used in select cases where long-term pain control is required.
In both cases, the medication is delivered intrathecally (into the fluid-filled space around the spinal cord) or epidurally (around the spinal cord), allowing it to act quickly on the nerves that transmit pain signals.
Risks and Considerations
While pain pumps offer clear advantages, they are not without potential drawbacks. Common risks include:
- Infection: Any device inserted into the body carries a risk of infection, particularly if the catheter site is not properly managed.
- Catheter displacement: Movement or improper placement of the catheter can result in inadequate pain control or medication leakage.
- Overdose or underdose: Improper programming or patient misuse may result in too much or too little medication delivery.
- Allergic reaction or drug sensitivity: Some patients may react to the medications used in the pump, requiring a change in drug formulation.
Close monitoring and clear patient education can minimize these risks. Most hospitals have strict protocols in place to ensure pain pump safety, including regular checks by nursing staff and adjustments by anesthesiologists or pain specialists.
Integration with Multimodal Pain Management
Pain pumps are not used in isolation. They are part of a broader strategy known as multimodal pain management, which combines different therapies to maximize comfort and recovery. Alongside the pump, patients may receive:
- Acetaminophen or NSAIDs to manage general pain and inflammation
- Gabapentinoids for nerve-related discomfort
- Cryotherapy and physical therapy to address muscle soreness and stiffness
- Breathing and relaxation techniques to reduce stress-related pain responses
This integrated approach ensures that pain is managed from multiple angles, minimizing the need for high doses of any single intervention and supporting faster functional gains.
Patient Education and Involvement
Patient understanding is critical when using a pain pump, especially when it includes a PCA component. Before surgery, patients are taught how the device works, what sensations to expect and how to safely activate it if self-administered. Clear communication reduces anxiety and enhances satisfaction with the recovery experience.
Nurses and surgical teams regularly check the system, monitor pain levels and educate patients about when the pump can be removed and how pain can be managed afterward. Transitioning from the pump to oral medications is done gradually to ensure continued comfort.
Future Directions in Pain Pump Technology
Advances in pain pump technology continue to make these systems more effective and user-friendly. Features like programmable dosing, smart feedback sensors and improved battery life are expanding their role in both acute and chronic care settings.
Researchers are also exploring new drug formulations and delivery routes that may improve efficacy while reducing side effects. As spinal surgery protocols move toward faster discharge and home-based recovery, pain pumps that are safe and easy to manage outside the hospital could become more widely used.
In the future, we may see fully automated, personalized systems that adjust pain medication delivery in real-time based on patient feedback, movement levels and biological markers.







Comments